As the healthcare industry continues to prioritise infection control and patient safety, the demand for medical-grade equipment that can withstand rigorous cleaning protocols has never been greater. At FutureNova, we’re proud to announce that our iBioShield 10X iPad cases have undergone extensive testing and certification, proving their compatibility with Clinell Universal Wipes – a staple in hospital environments for disinfection.
Testing Method
Led by Clinell’s Materials Science Lead, the testing aimed to assess the resilience of our iPad cases against the harsh chemicals found in Clinell Universal Wipes. Two stages of testing were conducted: wipe testing and partial immersion testing, each designed to evaluate the cases’ durability and resistance to degradation.
Wipe Testing Results
During wipe testing, our Slimline iBioShield 10X iPad case underwent thorough cleaning, with the entire surface area wiped 10 times per day for 10 consecutive days – totalling 100 wipes. Impressively, our cases showed no signs of discolouration, swelling, cracking, or degradation.
Partial Immersion Testing Results
In the subsequent partial immersion testing, our cases were partially submerged in Clinell Universal liquid formulation for 24 hours. Despite exposure to the liquid, our cases remained unaffected, with no visible signs of damage or degradation. While minor residues were observed after drying, these were easily removable with water, leaving the cases pristine and ready for use.
Confirmation of Compatibility
The results of our testing confirm that FutureNova’s iBioShield 10X iPad cases are fully compatible with Clinell Universal Wipes, providing hospital workers with a reliable solution for infection control and device protection. With our cases, healthcare professionals can confidently clean and disinfect their iPads without compromising on durability or performance.
Join us in our commitment to revolutionise infection control. With our Clinell certified compatible iPad cases, you can prioritise patient safety, while ensuring the longevity of your equipment.
Versatility of Clinell Wipes
Clinell Wipes aren’t just limited to hospital settings; their versatility extends across a wide range of industries and environments. From offices to schools, gyms, and public transportation, Clinell Wipes are indispensable for maintaining cleanliness and preventing the spread of infections.
Whether it’s wiping down desks, equipment, door handles, or surfaces in high-traffic areas, Clinell Wipes provide a convenient and effective solution for disinfection. With their proven compatibility with FutureNova’s iBioShield 10X iPad cases, industries outside of healthcare can also benefit from the assurance of optimal cleanliness and hygiene. Discover the difference today and elevate your infection control protocols with FutureNova.
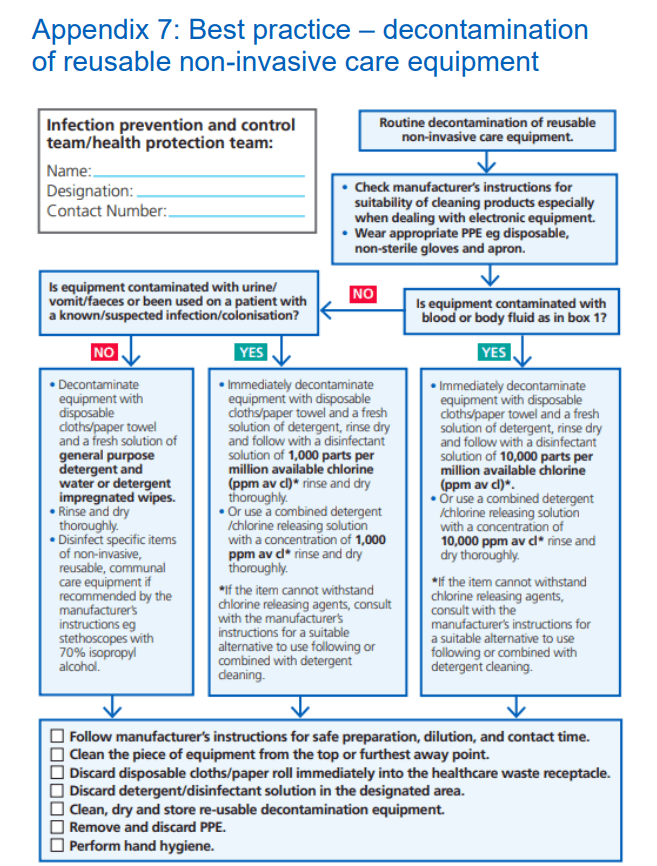
National Infection Prevention and Control Manual for NHS England
The NHS England best practice checklist, 2024, emphasises the importance of thorough decontamination, particularly for reusable non-invasive care equipment, such as our iPad cases.
Essential steps include wearing appropriate personal protective equipment (PPE), such as disposable non-sterile gloves and aprons, and conducting a comprehensive assessment of equipment for contamination with blood or body fluids. It also guides healthcare practitioners to adhere to manufacturers’ instructions regarding cleaning products, especially when handling electronic equipment.
In cases where contamination is confirmed, immediate decontamination is crucial, using a rigorous disinfectant solution containing a 10,000 ppm concentration of chlorine. This ensures effective eradication of harmful pathogens, safeguarding both patients and healthcare workers from potential infections.
Throughout the decontamination process, strict adherence to manufacturers’ instructions for safe preparation, dilution, and contact time is essential to ensure optimal efficacy. After completing the cleaning procedure, healthcare workers should discard any disposable materials and cleaning solutions appropriately and practice thorough hand hygiene to prevent the risk of cross-contamination.
By following these guidelines, healthcare facilities can maintain a hygienic environment and uphold stringent infection control standards, to enhance patient safety. The best practice guide can be viewed below:
(Credit: england.nhs.uk)


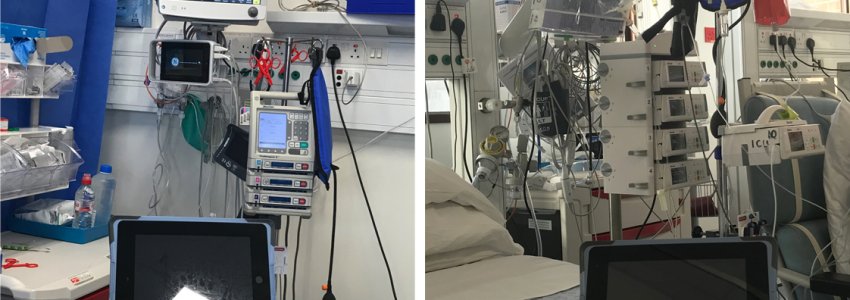



 Smart phones, tablets and other mobile devices are everywhere you turn in a modern healthcare facility, and although they can provide great benefits for how staff and patients interact with healthcare information, they can also provide homes for wandering pathogens.
Smart phones, tablets and other mobile devices are everywhere you turn in a modern healthcare facility, and although they can provide great benefits for how staff and patients interact with healthcare information, they can also provide homes for wandering pathogens.